Since launching our first eye drops, "ROHTO Eye Drops" in 1909, we have continued to respond to the changing eye concerns of our customers for over 100 years.
Initially developed as eye drops to treat a prevalent eye disease at the time, the product has continued to evolve in response to changing lifestyles and has since led the domestic eye care category. To address all of people's eye concerns, the company has developed not only eye drops, but also eye washes, contact lenses and their care products, and even supplements.
Currently, in addition to the over-the-counter (OTC) drugs we have developed so far, we are also developing prescription drugs. Furthermore, we are looking overseas and working to improve the eye health of people all over the world.
Going forward, as a total eye care company, we will continue to propose products that meet the evolving needs of our customers at various stages of health, preventative care, and illness, from daily care to disease treatment.
Research Case Studies
Eye strain in the digital age
The effects of blue light on corneal stem cells

corneal stem cells
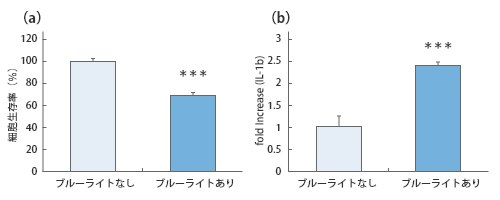
Changes in corneal stem cell viability (a) and gene expression levels of the inflammatory cytokine (IL-1b) (b) due to blue light irradiation.
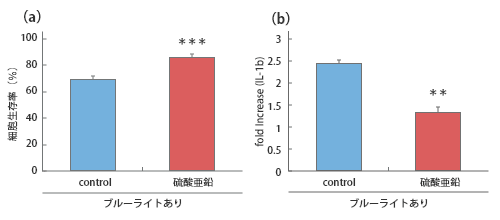
The effect of changes caused by blue light exposure on zinc nitrate hydrate
The rapid proliferation of digital devices has increased the amount of blue light that modern people are exposed to in their daily lives. Blue light is said to put a great strain on the eyes and body, and it has been suggested that it has various effects on the retina and cornea.
However, the impact on corneal stem cells, which produce new corneal epithelial cells daily and play a crucial role in corneal turnover and maintaining homeostasis, had not been clarified.
Therefore, we used a special device that can irradiate cells with blue light to investigate the effects of blue light on corneal stem cells.
The research revealed that irradiating corneal stem cells with blue light increased the expression of the inflammatory cytokine IL-1β, leading to a decrease in cell viability.
Furthermore, we discovered that zinc sulfate hydrate, the active ingredient in the eye drops, suppresses the increase in IL-1β expression and the decrease in cell viability, thereby protecting corneal stem cells from inflammation caused by blue light.
We will develop eye drops to alleviate eye discomfort caused by digital devices, which are expected to become even more widespread in the future.
Click here for more details.
A multifaceted approach to dry eyes
Dry eyes caused by friction when wearing contact lenses
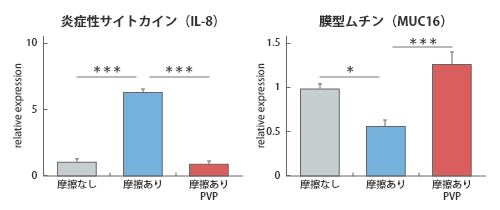
Changes in IL-8 mRNA expression levels/MUC16 mRNA expression levels due to frictional stimulation of cells and the effects of polyvinylpyrrolidone (PVP)
It is said that three things starting with "con"—contact lenses (CL), computers, and air conditioners—are involved in dry eyes.
One of the causes of dry eyes experienced when wearing contact lenses (CLs) is friction between the CL, cornea, and conjunctival surface that occurs when blinking. This friction is thought to irritate the eye and cause dryness when wearing CLs, but the detailed mechanism is not yet understood.
Therefore, we introduced a device that can apply a water flow load to corneal epithelial cells as a model of frictional stimulation, and conducted research to elucidate the mechanism by which friction stimulates the cornea.
The research revealed that friction stimulates an increase in the inflammatory cytokine IL-8 and decreases the expression level of MUC16, a membrane-bound mucin that helps retain tear fluid.
These results suggest that the mechanism by which friction causes dry eyes is that it causes inflammation on the cornea, reducing its wettability. Furthermore, we discovered that polyvinylpyrrolidone, the active ingredient in eye drops, suppresses the increase in IL-8 expression and the decrease in MUC16 expression caused by friction.
We will continue our research to develop eye drops that are effective in treating dry eyes when wearing contact lenses.
Development of formulation technology for forming a stable tear film
The tear film that covers the surface of the eye is composed of two layers: a water layer and an oil layer. When this tear film becomes unstable, it can cause eye discomfort such as dryness, pain, and fatigue.
Therefore, we began research to stabilize the "aqueous layer" and "oil layer" of tear film.
For a long time, surfactants have been used as "solubilants" to incorporate oily components into eye drops. On the other hand, in the formulation of skincare products, various technologies have been researched for the use of surfactants, including not only oil/water emulsification but also improving usability and penetration. Therefore, we considered whether these technologies and components could be adapted for eye drop development.
As a result, we identified the optimal type and ratio of surfactants for stabilizing tear film.
Instead of using it as a "solubilant" to dissolve oil, as in the conventional approach, incorporating it to "stabilize the tear film" after instillation has made it possible to develop eye drops that are ideal for people suffering from uncomfortable symptoms such as dryness.
Measures against hay fever and allergies
Research on allergic conjunctivitis
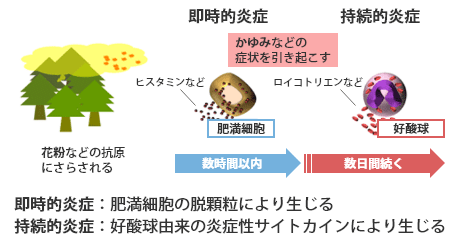
Two types of inflammatory mechanisms
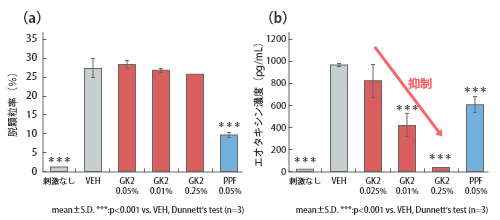
Changes in mast cell degranulation rate (a) and eosinophil inflammatory cytokine (eotaxin) production (b) under inflammatory conditions in GK2/PPF.
One of the causes of itchy and red eyes due to allergic conjunctivitis is inflammation caused by an allergic reaction to antigens such as pollen and house dust. Two types of inflammation are involved: "immediate inflammation," which occurs immediately after antigen exposure, and "persistent inflammation," which follows immediate inflammation.
The former occurs when mast cells that recognize an antigen undergo degranulation, while the latter occurs when eosinophils accumulate at the site of inflammation and release inflammatory cytokines.
Eye drops for allergic conjunctivitis contain several anti-inflammatory ingredients. One of these ingredients is dipotassium glycyrrhizinate (GK2), but the detailed mechanism of its anti-inflammatory action was not understood.
We confirmed that GK2 suppresses the production of the inflammatory cytokine eotaxin in human conjunctival fibroblasts under inflammatory conditions, such as when the cytokines IL-4 and TNFα are added, and discovered that it acts on persistent inflammation. We also found that pranoprofen is effective against immediate inflammation by suppressing degranulation.
Based on this knowledge, we are working on developing eye drops that are effective against allergic conjunctivitis.
Click here for more details.
The pursuit of the perfect eye drop application experience
Designed for ease of use and a focus on user comfort.
A container packed with attention to detail
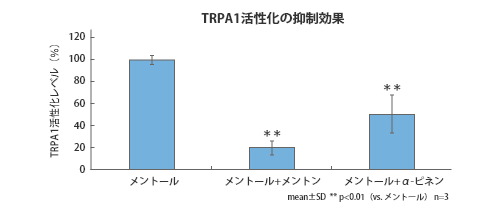
Results of searching for components that suppress pain receptors (TRPA1) activated by menthol
We strive to create products that our customers will enjoy using for a long time, focusing on ease of use and comfort.
To enhance ease of use, for example, our eye drops feature a "one-touch screw cap" that is easy to open and close, even for elderly people and children with weak fingers or hands; a "free-angle nozzle®" that allows eye drops to be dispensed from any angle, enabling comfortable use without tilting the head upwards; and our eye wash features an "easy cup®" that allows for thorough eye washing without having to tilt the head upwards.
On the other hand, an example of eye drops that prioritize user comfort is "Smart Cool Tech®," which quantifies the level of comfort it provides.
While eye drops contain menthol and other ingredients that provide a refreshing, cooling sensation when applied to the eye, some people have experienced irritation. Therefore, by focusing on "pain receptors," one of the sensory receptors on the surface of the eye, and researching and incorporating ingredients that inhibit their activation, we were able to develop eye drops that cause less irritation.
Click here for more details.
A new challenge: Aiming to "regenerate eyes"
Research on differentiation induction into corneal epithelial cells using iPS cells
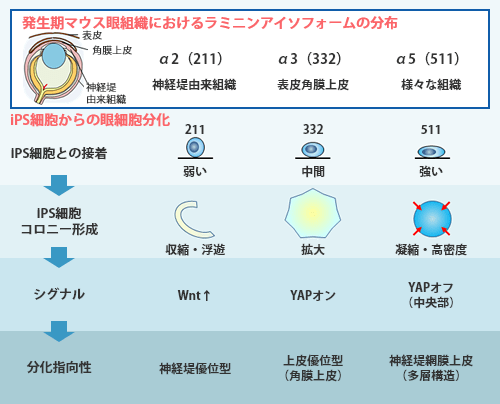
Using laminin isoforms, it is possible to control the differentiation of human iPS cells into various eye-related cells.
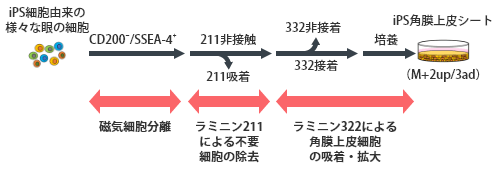
By utilizing the cell-specific adhesion properties of laminin isoforms, corneal epithelial cells derived from human iPS cells can be purified.
iPS cells, first created in 2006, are a type of pluripotent stem cell that can differentiate into almost any cell type. Compared to ES cells, another type of pluripotent stem cell derived from fertilized eggs, iPS cells have resolved ethical issues, and in recent years, particularly in Japan, clinical trials have been conducted to transplant cells and tissues derived from iPS cells into patients as Regenerative medicine to treat diseases.
In collaboration with Osaka University, we have been conducting research on the differentiation induction of iPS cells into eye-related cells, particularly corneal epithelial cells.
Previously, we revealed that the type of laminin, a basement membrane protein used to coat culture dishes, contributes to the fate determination of iPS cells during their differentiation into eye cells. This finding is expected to elucidate the mechanisms of iPS cell fate determination controlled by the scaffold, the developmental mechanisms of the eye, and improve the efficiency of iPS corneal epithelial cell production for the practical application of corneal Regenerative medicine.
Furthermore, we have established a new method for purifying corneal epithelial cells from a cell population containing various eye cells derived from iPS cells. This achievement is expected to facilitate the widespread adoption of iPS corneal epithelial cell sheet transplantation therapy and simplify, streamline, and reduce the costs of isolating iPS corneal epithelial cells and manufacturing cell sheets for industrial applications.
Click here for more details.